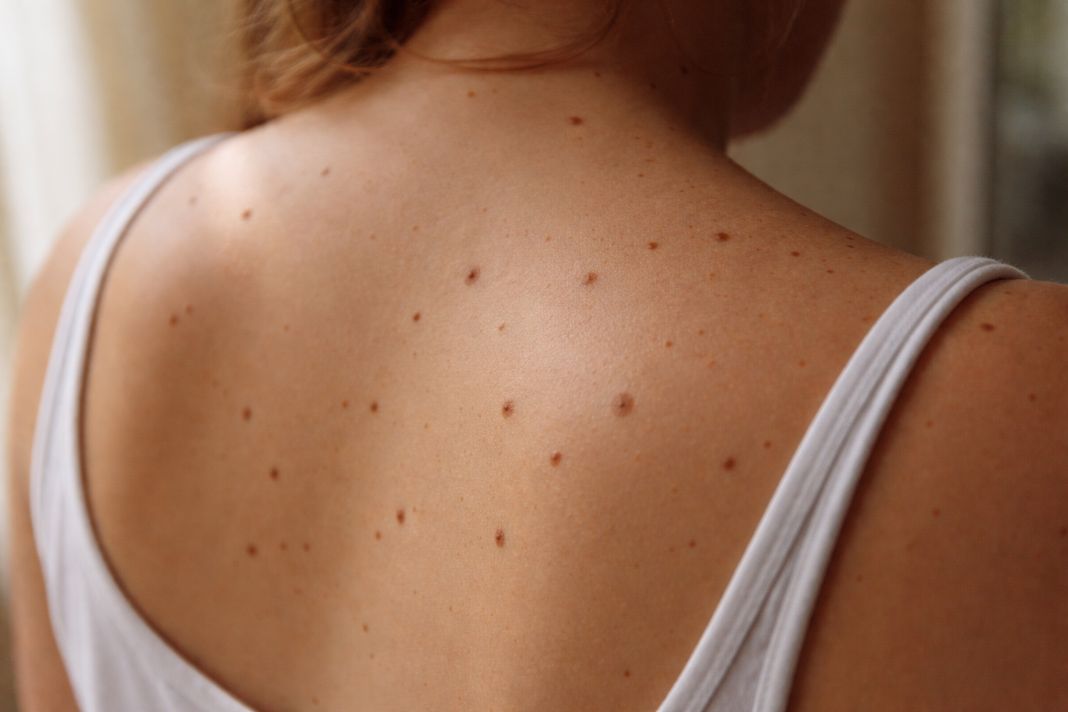
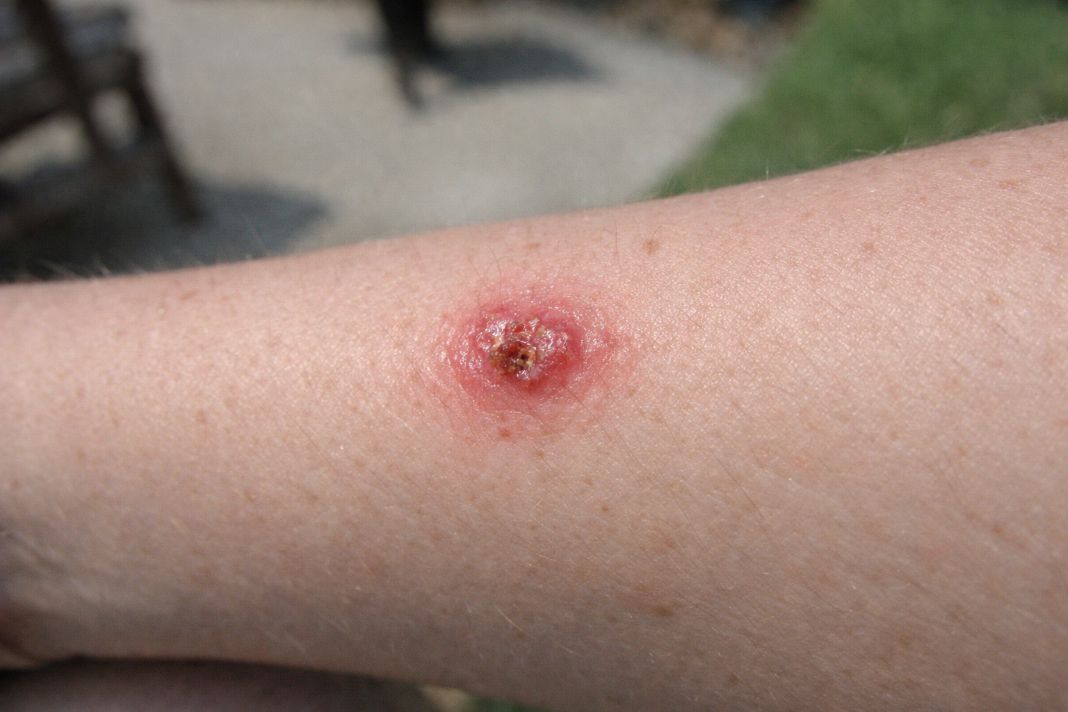
How often should you get a skin check, and does age affect the timing?
Skin check frequency depends on your personal risk, not on age alone. Many people can monitor their skin at home and arrange a professional review if something changes, while others need regular dermatologist-led checks because of factors such as family history, previous skin cancer, heavy sun exposure, or a large number of moles. Age does affect risk because sun damage builds up over time, but the right interval is always based on the full picture.
What Is In This Article
Why skin checks matter: early detection and risk factors
A new mole, a patch that will not heal, or a mark that starts to change can be easy to dismiss at first. Skin checks matter because they turn those small observations into a structured review, which can identify harmless changes as well as lesions that need closer attention.
Skin cancer screening is a medical issue, not a cosmetic one. Melanoma and other skin cancers can look subtle in the early stages, and some non-cancerous growths can look worrying without expert assessment. Guidance from the NHS, NICE guidelines and the British Association of Dermatologists supports the principle of paying attention to suspicious skin changes and assessing risk in context.
Self-examination and professional checks do different jobs. A self skin check helps you notice change over time in your own body. A dermatology check by a clinician adds training, pattern recognition and tools such as dermatoscopy, which allows a closer look at pigment and structure beneath the surface.
Several factors make regular skin health monitoring more important:
- A personal history of skin cancer or pre-cancerous lesions
- A family history of melanoma
- Fair skin that burns easily, although darker skin does not remove risk
- A high number of moles, unusual moles, or changing lesions
- Repeated sunburn, including in childhood
- Frequent sun exposure through work, sport, or travel
- Use of tanning beds
Occupational and environmental exposure can matter as much as skin type. Someone who works outdoors, spends weekends sailing, or travels often to high-UV climates may need a different screening pattern from a person with similar skin who has far less cumulative exposure. Consultant dermatologists usually look at these details together, because risk builds from a combination of factors rather than one simple label.
How age influences skin check frequency
Age changes the background level of risk because the skin carries the record of previous sun exposure. That does not mean every older adult needs the same screening interval, and it does not mean younger adults are automatically low risk.
A practical way to think about skin check by age is to treat age as one part of a wider risk profile:
| Age group | General pattern |
|---|---|
| Teens and 20s | Professional checks are often based on symptoms, mole changes, family history, or high sun exposure rather than routine annual review |
| 30s and 40s | Risk assessment often becomes more relevant, especially if there is cumulative sun damage, many moles, or a history of blistering sunburn |
| 50s and over | Professional review may be advised more often because cumulative sun exposure, age-related skin change, and skin cancer risk all become more relevant |
A healthy 25-year-old with no family history, no suspicious lesions and little history of sun damage may only need self-monitoring and prompt review of any new or changing mark. By contrast, a 55-year-old with fair skin, outdoor hobbies and numerous moles may be advised to have regular professional skin assessment even if nothing currently looks alarming.
Childhood sunburn still matters later in life. Skin damage from earlier decades can influence adult risk, which is one reason age and skin cancer risk are linked even when a person now works indoors and uses sun protection more consistently.
Older skin also develops benign changes such as seborrhoeic keratoses, cherry angiomas and sun spots. Those can mimic more serious lesions to the untrained eye, which is why age-specific dermatology advice often focuses on pattern recognition as much as on simple frequency.
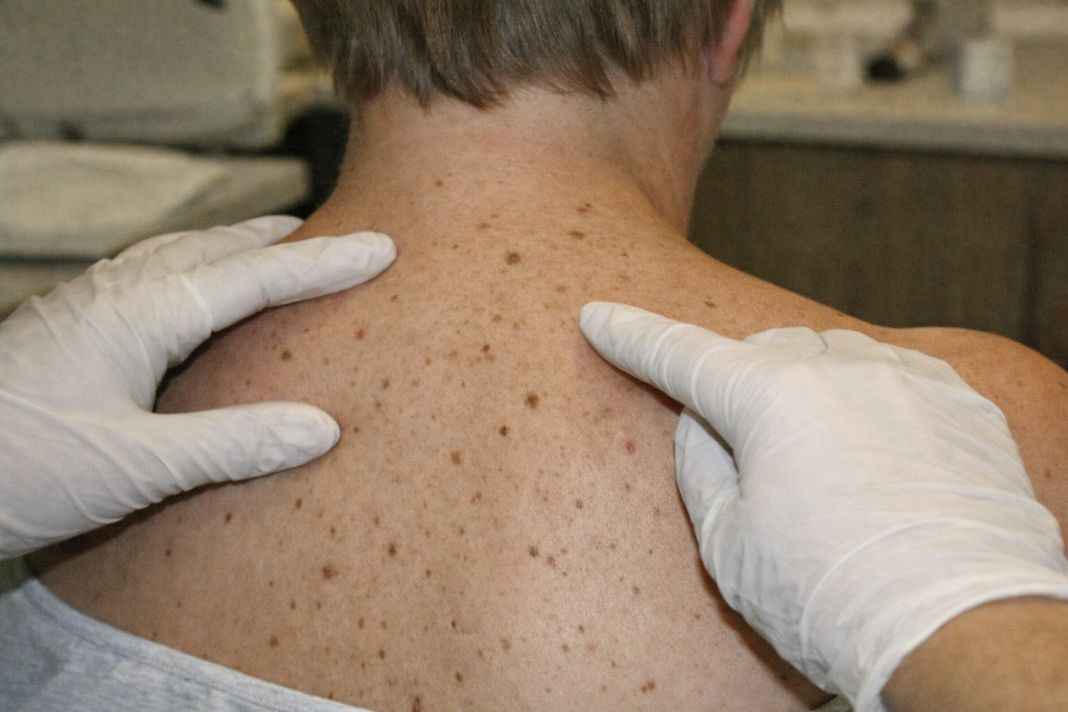
Skin examination – Illustrative Image
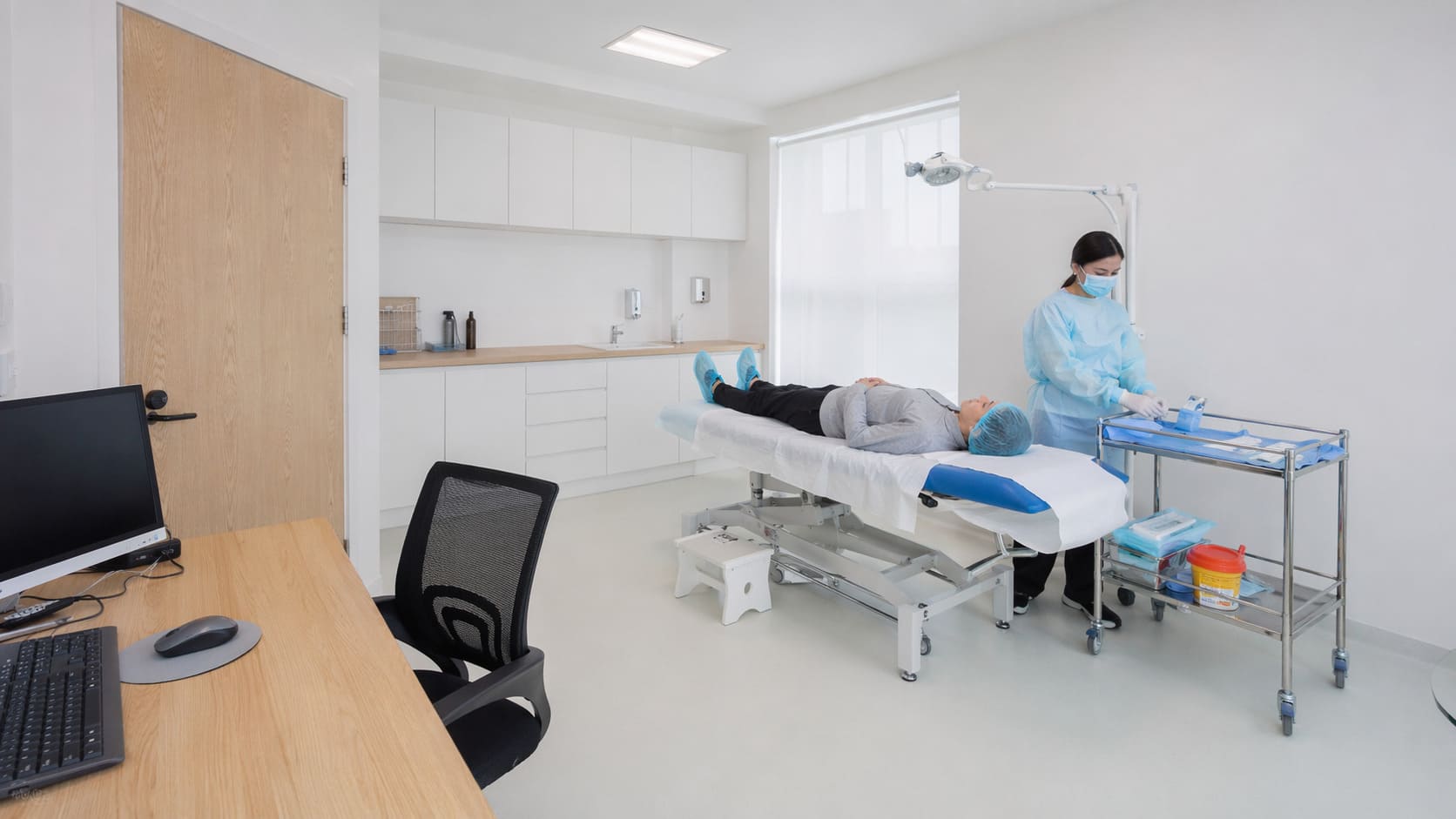
What happens during a professional skin check?
A professional skin check is a structured clinical examination. The aim is to review your skin systematically, identify any lesions that need closer attention, and decide whether monitoring, imaging, biopsy or treatment is appropriate.
At Future Care Medical, a dermatology consultation follows a clear process rather than an informal visual glance.
- The appointment usually begins with a short medical history. The clinician asks about previous skin cancer, family history, recent mole changes, symptoms such as itching or bleeding, and patterns of sun exposure.
- The examination then focuses on the area of concern or, if indicated, a wider full-body examination. Privacy is maintained throughout, and patients can raise any lesions they have noticed.
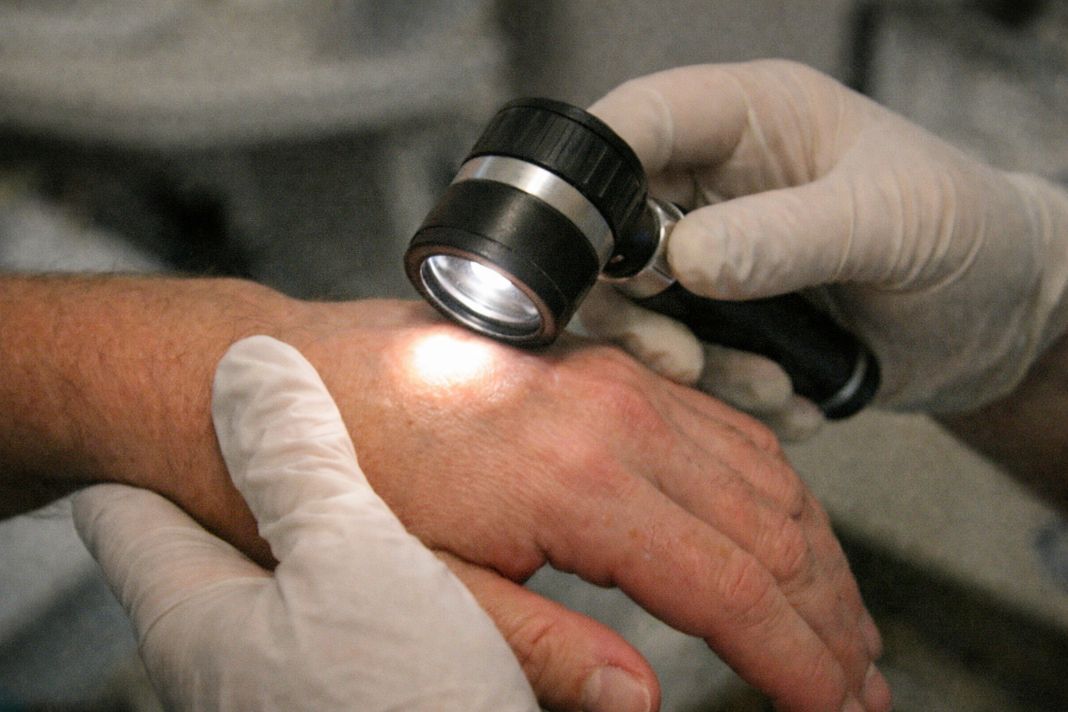
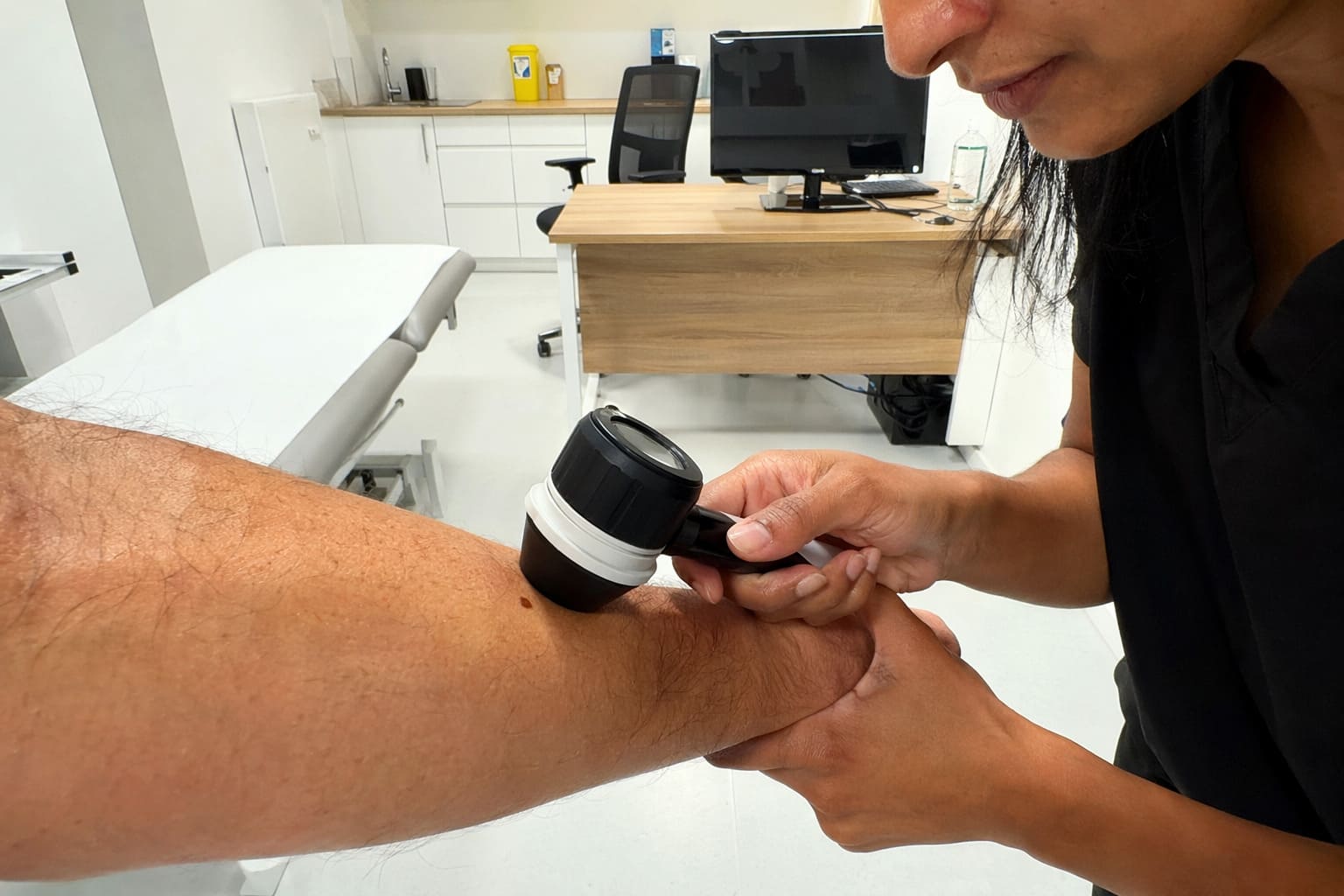
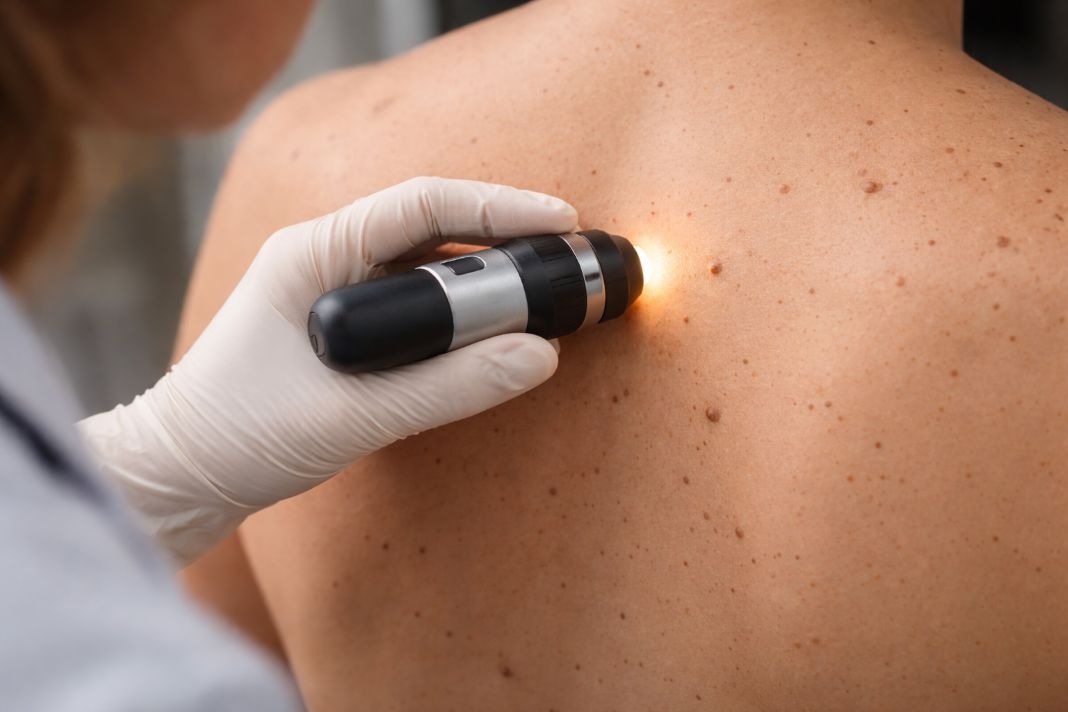
- A dermatoscope may be used to assess pigment patterns and surface structures in more detail. This helps distinguish lesions that appear similar to the naked eye.
- If monitoring is needed, lesion documentation or clinical photography may be used. Mole mapping can be useful in selected cases where tracking change over time is part of the plan.
- The findings are explained clearly. Some lesions are confidently benign, some require follow-up, and others may need biopsy or removal to confirm a diagnosis.
Comfort and privacy are part of the appointment design. Patients are usually told which parts of the skin need to be examined, why that matters, and what the next clinical step is if something suspicious is found.
Sometimes the outcome is simple reassurance based on a benign lesion with stable features. In other cases, the value of the review lies in documenting a mark that does not need treatment now but should be compared at a later date.
Self-examination vs. Professional assessment: what is the difference?
A self skin check is useful for spotting change early, but it cannot diagnose skin cancer. A professional skin assessment adds clinical training and diagnostic tools, which means that the two approaches work best together.
| Self-examination | Professional assessment |
|---|---|
| Helps you notice new or changing marks between appointments | Assesses lesions in a structured clinical setting |
| Can be done regularly at home | Includes dermatoscopic review where appropriate |
| Depends on what you can see and recognise | Identifies patterns that are easy to miss without training |
| Useful for tracking symptoms such as bleeding or itching | Guides follow-up, biopsy, removal, or discharge |
For a practical mole self-exam, the British Association of Dermatologists and NHS advice broadly supports looking for change in size, shape, colour and sensation. The ABCDE rule is often used as a guide: asymmetry, border irregularity, colour variation, diameter, and changing change.
A simple home routine can include:
- Check your skin in good light once a month.
- Use a mirror for hard-to-see areas, including the back, scalp and backs of the legs.
- Take clear photos if a mole or lesion is being watched over time.
- Note bleeding, crusting, itching, pain or rapid change.
Phone photos and tracking apps can help with lesion monitoring, but they have limits. Image quality varies, and a photograph cannot replace examination with a dermatoscope or clinical judgement about whether a lesion needs biopsy.
Any mole or skin lesion that changes noticeably, bleeds without obvious injury, does not heal, or starts to look different from surrounding marks deserves professional review. That applies even if the lesion is small, because early lesions are not always dramatic in appearance.
Dermatoscope Mole Review – Illustrative Image
How location and lifestyle affect skin check needs
A City of London office worker may assume that skin cancer risk belongs mainly to people who spend all day outdoors. Daily life is usually more mixed than that. Commuting, weekend sport, holidays, rooftop lunches, gardening and repeated travel to sunnier climates all add up over time.
Lifestyle risk is often cumulative rather than obvious. Someone based near Liverpool Street or Moorgate may spend weekdays indoors but take frequent skiing or Mediterranean holidays, run outdoors at midday, or have a long history of tanning in earlier years. Those details can shift skin check frequency more than a postcode ever will.
Relevant lifestyle and location factors include:
- Outdoor work, construction, sport coaching, or regular exercise in direct sun
- Frequent travel to high-UV regions
- Previous use of sunbeds
- Inconsistent use of sunscreen or protective clothing
- A history of repeated sunburn
- Long periods spent near reflective surfaces such as water, snow or sand
Urban living does not remove UV exposure. City residents often underestimate incidental sun, particularly during spring and summer when exposure happens in shorter bursts. British Association of Dermatologists guidance on sun protection and UV awareness is therefore relevant to office workers as well as outdoor staff.
For people working in Central London, access can affect whether concerns are assessed promptly. A clinic such as Future Care Medical, based on London Wall, may be convenient for those moving between Bank, Bishopsgate, Moorgate and the wider Zone 1 area, but convenience does not replace risk assessment. Screening intervals still need to reflect your history, habits and skin findings.
What does a skin check cost in Central London?
In private practice, the cost of a skin check in Central London depends on who carries it out, how long the appointment lasts, and whether the visit covers a focused mole check or a wider dermatology consultation.
At Future Care Medical, a 60-minute GP consultation is listed at £240.00, and that may be relevant where an initial medical review of a skin concern is appropriate. If a consultant dermatologist skin check is being arranged, fees depend on the specialist consultation structure and any follow-up investigations or procedures required.
What is usually included in a professional skin assessment fee can vary, but commonly covers:
- Review of medical history and risk factors
- Examination of the lesion or wider skin area
- Use of dermatoscopy where indicated
- Explanation of findings and recommended next steps
Biopsy, lesion removal, pathology and follow-up review are usually separate items if they are needed. Patients using private health insurance should check whether dermatology consultations, diagnostics and minor procedures are covered under their policy, because insurer terms differ. Self-pay patients often want clarity on whether the appointment is diagnostic only or whether treatment could be discussed at the same visit.
Skin Lesion Removal Procedure – Illustrative Image
Common misconceptions about skin checks and age
Several myths still shape how people think about skin screening facts, and some of them lead to delay.
Myth: Only older adults need skin checks. Fact: Risk often rises with age, but younger adults can still develop melanoma or other skin cancers, especially if they have strong risk factors such as family history, many moles or significant UV exposure.
Myth: If I check my own moles, that is enough. Fact: Self-monitoring is useful, but it does not replace professional assessment when a lesion is changing or hard to interpret.
Myth: Darker skin means no risk. Fact: Skin cancer is less common in some darker skin types, but it can still occur. Delayed recognition can be a problem if people assume they are fully protected.
Myth: Indoor work means I do not need to think about sun damage. Fact: Cumulative exposure from commuting, holidays, outdoor exercise and earlier life habits still matters.
Myth: Everyone should have a skin check every year. Fact: There is no single interval that fits everybody. Frequency depends on personal history, skin type, mole pattern, age, sun exposure and any previous abnormal findings.
Public health campaigns and NHS messaging usually focus on warning signs and risk awareness because confusion often comes from oversimplified rules. A person in their thirties with many atypical moles may need closer review than a person in their sixties with very low risk and no suspicious lesions, which shows why assumptions can be misleading.
Looking ahead: changing guidance and personal risk assessment
Skin screening is moving further toward risk-based advice. NICE, the British Association of Dermatologists and other clinical bodies continue to shape guidance around symptoms, referral thresholds and assessment pathways, but personal risk stratification is becoming more central to how follow-up is planned.
That means the future of skin checks is unlikely to rest on age alone. A patient’s mole pattern, previous pathology, sun exposure history, skin type, family history and ability to monitor change all contribute to a more individual schedule.
Diagnostic tools may continue to improve how lesions are documented and compared over time, including dermatoscopic imaging and structured photographic monitoring in selected cases. Even so, the underlying principle is unlikely to change: the best timing for a skin check is the timing that matches your actual risk, your current skin findings and any new changes you notice.
A sensible approach is to treat skin health as something that needs periodic review, much like blood pressure or vision. Risk can shift across the decades, and the right answer at 25 may not be the right answer at 55.