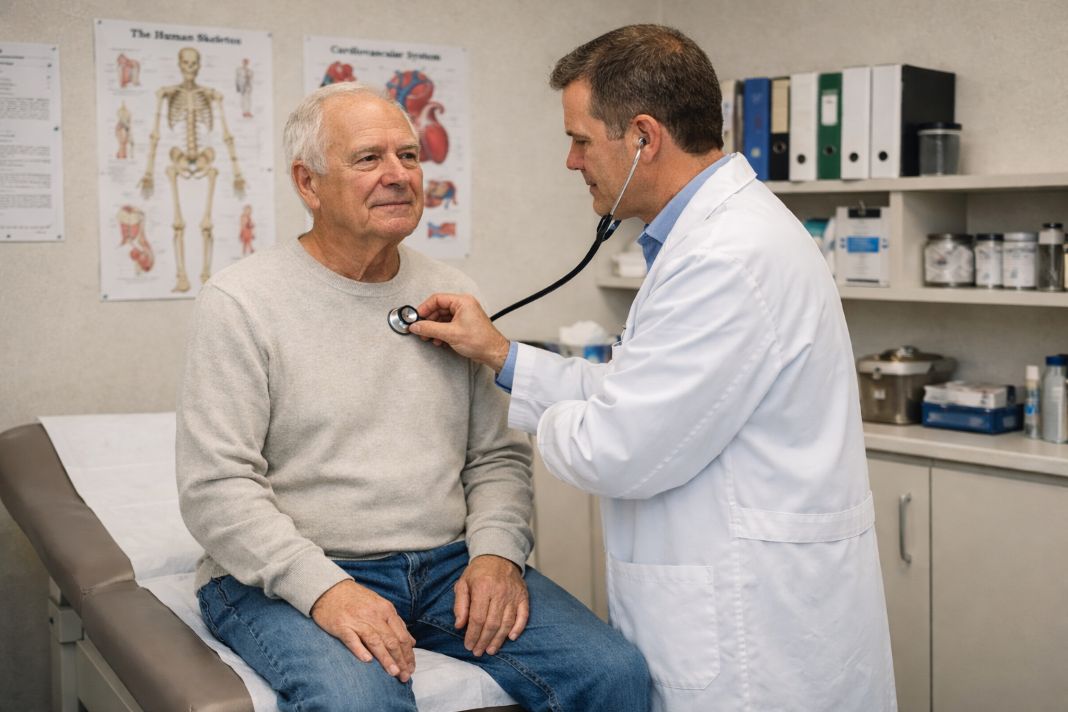
What does a cardiovascular risk assessment tell you, and when is it worth having one?
A cardiovascular risk assessment estimates the likelihood of a future heart or circulatory problem by looking at a range of factors such as blood pressure, cholesterol, age, smoking status, diabetes risk and family history. It is usually worth considering when age, medical history, ethnicity, lifestyle or existing risk factors suggest that a structured heart health check could give a clearer picture than symptoms alone.
Here's What We Have Covered In This Article
Understanding Cardiovascular Risk Assessment
A cardiovascular risk assessment is a way of estimating risk over time. It does not confirm that someone has heart disease, and it does not rule it out with certainty. Instead, it brings together personal and clinical information to produce a more informed prediction of the chance of a cardiovascular event, such as a heart attack or stroke, within a defined period.
That distinction matters. Diagnosis looks for evidence of a condition that is already present. Risk assessment looks ahead. In practice, it works more like a weather forecast than a snapshot. A forecast cannot promise what will happen on one specific day, but it can show whether the conditions make a storm more likely.
Feeling well does not always reflect underlying cardiovascular risk. High blood pressure and raised cholesterol often cause no obvious symptoms, which means that someone may feel fit, exercise regularly and still carry a higher risk than expected. Public guidance from bodies such as the NHS, NICE and the British Heart Foundation reflects that reality by focusing on measurable risk factors rather than appearance or self-perception.
Structured tools are used because guesswork is unreliable. Clinicians may use calculators such as QRISK in the UK, and some settings may also refer to models such as the Framingham Risk Score. These tools are based on recognised risk factors for heart disease, which means that the final estimate is grounded in patterns seen across large populations rather than intuition alone.
A heart disease risk assessment often includes:
- blood pressure
- cholesterol and other blood lipid results
- age, sex and ethnicity
- smoking status
- diabetes status or diabetes screening
- family history
- weight or BMI
- lifestyle assessment, including activity levels and alcohol intake
Pro Tip: If you have a family history of early heart disease, highlight this during your appointment as it can significantly affect your risk calculation.
Schedule Your Heart Health Check
Book a private cardiovascular risk assessment at Future Care Medical for a thorough review of your heart health and actionable next steps.
What Does a Cardiovascular Risk Assessment Involve?
A cardiovascular screening process usually follows a clear sequence, starting with history and basic measurements before any risk score is calculated. Some people complete a quick online self-assessment first, but an in-clinic cardiac risk evaluation is broader because it combines personal answers with examination and blood testing.
A typical appointment may include the following steps:
- A clinical consultation covering medical history, medicines, family history and lifestyle.
- Physical measurements such as blood pressure, weight and BMI.
- Blood tests, commonly including a cholesterol test and blood lipid profile.
- Review of smoking status, diabetes risk and any existing conditions.
- Calculation of risk using a validated tool such as a QRISK calculator.
- Discussion of the results and any follow-up plan.
During the consultation, a GP or nurse practitioner will usually ask about details that can affect long-term cardiovascular risk. Those details may include whether close relatives had early heart disease, whether you smoke now or did so in the past, and whether you have conditions such as high blood pressure or diabetes.
Measurements taken in clinic add another layer of accuracy. Blood pressure readings, height, weight and waist-related patterns can all shape risk. Blood tests for heart risk commonly look at total cholesterol, HDL cholesterol and sometimes broader metabolic markers depending on the setting.
Some assessments include further tests when there is a clinical reason to do so. An ECG, for example, may be used if symptoms, examination findings or medical history suggest that a simple risk score does not tell the full story. A standard risk assessment does not always require one.
At Future Care Medical, the process can sit within a wider private heart check or broader health screening pathway, depending on what is clinically relevant. That point is worth noting because a cardiovascular assessment can be a standalone review or one part of a more full health check.
Who Should Consider a Cardiovascular Risk Assessment?
Timing depends on personal risk, not on a single universal age. Some people are invited for cardiovascular checks through routine primary care pathways, including NHS health check programmes in midlife, but others may need earlier review because their background places them in a higher-risk group.
Age remains one of the strongest drivers of heart screening age decisions. Even so, younger adults may still need assessment if they have raised blood pressure, diabetes, a strong family history of early heart disease, or certain ethnic backgrounds associated with higher cardiovascular risk.
Work patterns can also influence when to have a cardiovascular check. People in demanding jobs across the City of London, Bank, Moorgate or Liverpool Street may spend long hours sitting, sleeping poorly, eating irregularly or carrying sustained stress. None of those factors alone proves a problem, but they can sit alongside blood pressure, lipid changes and weight gain in a way that justifies review.
The people most likely to benefit include:
- adults invited for routine midlife cardiovascular screening
- anyone with a family history of premature heart disease or stroke
- people with high blood pressure, raised cholesterol, diabetes or prediabetes
- smokers and former smokers with other risk factors
- individuals from higher-risk ethnic groups where earlier assessment may be appropriate
- adults with obesity, low physical activity or persistent metabolic concerns
NICE guidance supports risk-based prevention, which means that early detection matters most when a person has enough background risk for intervention to be useful. A healthy-looking person with hidden hypertension may need assessment sooner than an active person of the same age with no relevant history.
For central London professionals seeking a structured review that fits around work, private clinics such as Future Care Medical are one route into that assessment process. In many cases, the key issue is less about where the check happens and more about whether the decision to have one is based on identifiable risk.
Interpreting Results and What Happens Next
Results are usually explained in plain terms after the relevant information has been gathered and the score calculated. A clinician will normally discuss what your cardiovascular risk results mean, which factors are fixed, and which can be changed.
Risk categories vary according to the tool being used and the clinical setting, but the discussion often follows a simple pattern:
- lower estimated risk, where routine monitoring and lifestyle review may be enough
- intermediate estimated risk, where closer follow-up or added testing may be considered
- higher estimated risk, where medication, further investigation or structured prevention becomes more likely
Non-modifiable factors include age, sex, ethnicity and family history. Modifiable factors include smoking, blood pressure, cholesterol, weight, physical activity and some aspects of diabetes control. That distinction helps make an abstract score more practical, because the conversation then shifts from percentage alone to the areas where change is possible.
One person with a moderate score may be advised to repeat blood pressure checks, improve diet, increase activity and arrange follow-up screening after a set interval. Another may need medication alongside lifestyle changes if blood pressure or cholesterol levels are already significantly raised. A score is therefore a starting point for decisions, not the whole decision itself.
Follow-up often happens in primary care or in a private clinic, depending on how the assessment was arranged. At Future Care Medical, a 15-minute GP consultation costs £105, which may be relevant if a patient needs a focused review of blood results, blood pressure readings or medication options after an initial screening appointment.
Pro Tip: Bring a list of your medications and any recent blood test results to your assessment for a more complete risk review.
Common Misconceptions About Cardiovascular Risk Assessment
Misunderstandings are common because the phrase sounds more definitive than it is. A risk assessment is useful, but it has limits, and clear expectations matter.
Myth: If I feel fine, I do not need a heart health check. Fact: Many cardiovascular risk factors are silent. High blood pressure and raised cholesterol may cause no symptoms for years.
Myth: A normal score means I will not develop heart disease. Fact: Risk tools estimate probability, not certainty. They reduce uncertainty, but they do not eliminate it.
Myth: One blood test tells me everything about my heart. Fact: Cholesterol is important, yet it is only one part of a multi-factorial assessment that also includes blood pressure, diabetes risk, smoking and family history.
Myth: Lifestyle alone determines my result. Fact: Lifestyle matters greatly, although inherited factors, age, sex and ethnicity can also influence the final score.
Myth: Cardiovascular screening is the same as diagnosis. Fact: Screening and risk prediction identify likelihood and prompt further steps where needed. They do not confirm blocked arteries, rhythm problems or other specific conditions on their own.
British Heart Foundation messaging and public health campaigns often stress the same point: prevention works best when risk is identified before symptoms appear. Equally, NICE-based assessment tools are population guides, which means that clinical judgement still matters for the person sitting in front of the GP or nurse.
The Changing Role of Cardiovascular Risk Assessment in Preventative Health
Preventative heart care is becoming more precise. Risk prediction tools continue to be refined as evidence improves, and digital health platforms now allow some people to track blood pressure, pulse patterns and activity levels between appointments.
Remote monitoring can add useful context when used properly. Home blood pressure readings, wearable data and repeat measurements over time may show patterns that a single clinic visit misses. Even so, those data are most useful when interpreted alongside standard clinical information rather than in isolation.
Personalised risk prediction is also receiving more attention. Future versions of cardiovascular screening may incorporate a wider range of markers and better account for individual variation, particularly in groups whose risk has sometimes been under-recognised by older models.
Across central London and beyond, the broader shift is clear: prevention is moving earlier, becoming more data-informed and relying less on symptoms as the first signal that something is wrong. For patients, the practical takeaway is simple. A cardiovascular risk assessment is best seen as part of ongoing health planning, reviewed at the right time and interpreted in context rather than treated as a one-off verdict.
Discuss Your Results with a GP
If you have had recent blood tests or risk assessments, arrange a focused consultation with our experienced GPs to interpret your results and plan your care confidently.