What is the difference between exosomes and polynucleotides, and how does a doctor choose between them?
Exosomes and polynucleotides are two doctor-led regenerative skin treatments used in medical aesthetics. They differ in how they work, what tissue response they aim to support, and which clinical concerns they are best suited to address. A doctor chooses between them by assessing skin quality, treatment goals, medical history, suitability, and the need for monitoring within a structured clinical pathway.
Here's What We Have Covered In This Article
Understanding Exosomes and Polynucleotides in Clinical Practice
Exosomes and polynucleotides are often discussed together because both sit within the area of regenerative medicine and non-surgical interventions. Even so, they are not the same treatment and should not be treated as interchangeable options.
Exosome therapy refers to treatment based on microscopic extracellular vesicles involved in cell signalling. Polynucleotide injections use purified chains of nucleotides, which are building blocks associated with DNA and RNA, to support tissue repair and hydration within the skin.
In medical aesthetics clinics, these treatments are generally considered for skin quality improvement rather than simple volume replacement. That point matters because they differ from more familiar injectables such as dermal fillers, which are used mainly to restore shape or contour, and from topical products, which act at a more superficial level.
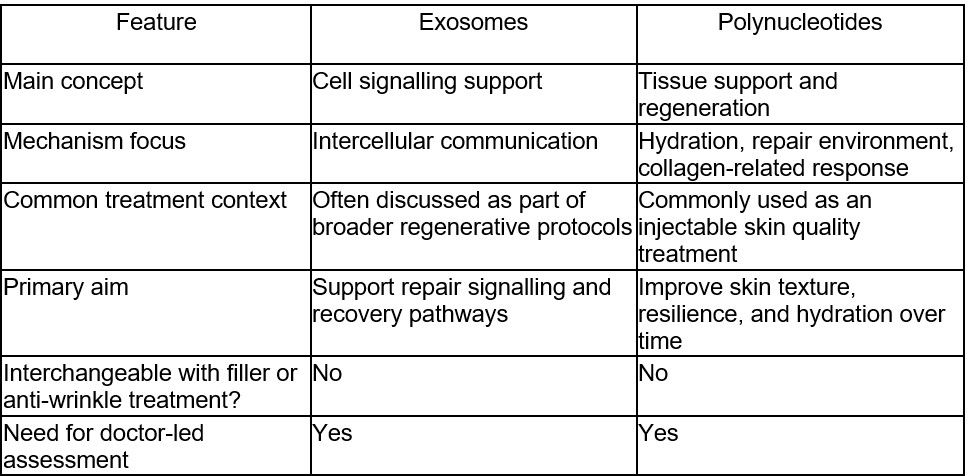
A straightforward way to separate them is this:
- Exosomes are discussed in relation to cell-to-cell communication and tissue repair signalling.
- Polynucleotides are discussed in relation to tissue support, hydration, and regenerative response within the skin.
- Both are doctor-led skin procedures that require assessment, suitability checks, and clinical oversight.
Across a central London clinical practice, interest in these treatments has grown because many patients want options that focus on skin function and tissue health, including texture, recovery, and overall skin quality, without moving straight to more invasive procedures.
How Exosomes Work: Mechanism and Clinical Applications
Exosomes are tiny vesicles released by cells. Their significance lies in the biological messages they can carry, including signalling molecules involved in communication between cells.
In clinical terms, the exosome mechanism is usually explained through cell-to-cell communication. Instead of acting as a filler or a surface treatment, exosome skin treatment is considered for how it may influence tissue repair processes and local skin behaviour through signalling pathways.
One useful way to think about exosome-based therapies is to picture them as biological messengers. That comparison is simplified, but it captures the central idea that the treatment is related to communication within tissue rather than mechanical support.
Clinical exosome application is commonly discussed in settings where a doctor is considering skin recovery, skin quality, or adjunctive use alongside other procedures. Depending on protocol, exosomes may be applied after procedures intended to create controlled stimulation in the skin. In some settings, they are also considered in scalp-related care, although the exact use depends on clinical governance and product selection.
Safety and oversight deserve close attention here. Exosome safety is not simply a question of whether a treatment is injected or applied. Product origin, manufacturing controls, storage, handling, indication, and regulatory standards all matter. A doctor therefore needs to review the source of the treatment, the intended use, and whether that use sits within appropriate medical regulatory standards.
Some misconceptions arise because the term sounds advanced and is sometimes used loosely. Exosomes are not a shortcut to guaranteed regeneration, and they are not a generic add-on that suits every patient. Their place, where used, should sit within clinical protocols with proper consent and safety monitoring.
Pro Tip: Pre-treatment photography helps track subtle improvements in skin quality over time and supports a more objective assessment.
Book a Clinical Consultation
Schedule a personalised assessment to find out which regenerative skin treatment is right for you.
How Polynucleotides Work: Mechanism and Clinical Applications
Polynucleotide therapy is usually framed around tissue repair support, hydration, and skin regeneration injections that aim to improve skin quality over time. The material used consists of purified nucleotide chains, and the treatment is generally delivered by injection into specific areas after a doctor-led assessment.
From a biological point of view, the polynucleotide mechanism is linked to creating a more supportive tissue environment. Doctors may discuss collagen stimulation, improved hydration, and support for repair processes within the skin. The emphasis is usually on skin quality rather than lifting, filling, or freezing movement.
Unlike fillers, polynucleotide injectables are not primarily used to add structure. Unlike anti-wrinkle injections, they are not intended to reduce muscle activity. Their role within advanced medical aesthetics is different, which means that treatment planning has to start with the actual concern being addressed.
Clinical polynucleotide use is often considered in areas where the skin is thin, tired-looking, or showing signs of reduced resilience. Under-eye skin, the face, neck, and hands may all be discussed depending on the product and the patient profile. Suitability still depends on factors such as inflammation, active skin disease, allergies, infection risk, and the wider medical history.
Patient selection criteria are central. If a person wants immediate contour change, a regenerative injectable may not match that goal. If the concern is skin texture, hydration, or gradual improvement in skin quality, polynucleotides may be part of the discussion.
Comparing Exosomes and Polynucleotides: Key Differences
Doctors compare exosomes vs polynucleotides by looking at mechanism of action, indication, delivery method, and treatment objective. The difference between exosomes and polynucleotides becomes clearer once the focus shifts from marketing language to clinical reasoning.
One treatment is not automatically stronger, newer, or better than the other. A patient comparing exosome or polynucleotide treatment needs to understand that they may be chosen for different reasons, even when the broad goal sounds similar.
Suitability also varies. Exosomes may be considered where signalling and procedural support are part of the treatment plan. Polynucleotides may be considered where the doctor wants a direct injectable approach aimed at skin regeneration and hydration in a defined area.
Expected outcomes differ in character as well. Regenerative treatment options are usually discussed in terms of gradual change in skin quality, not dramatic overnight transformation. In a London-based clinical practice, that distinction is often important for professionals who want realistic timelines and a clear explanation of what a treatment is actually intended to do.
How Doctors Decide: Clinical Assessment and Treatment Selection
Choosing exosomes or polynucleotides starts with assessment, not preference. A doctor looks at the skin concern itself, the treatment goal, the condition of the tissue, and whether the patient is medically suitable for the proposed plan.
At Future Care Medical, that process sits within structured treatment pathways rather than a menu-style approach. The question is not which treatment sounds more advanced. The real issue is which option, if either, fits the clinical picture.
A consultation commonly covers the following points:
- Medical history, including skin disease, allergy history, autoimmune issues, medication use, and previous procedures.
- Examination of skin quality, inflammation, pigmentation, laxity, scarring, hydration, and barrier condition.
- Clarification of goals, including whether the patient wants improved texture, recovery support, or a different type of result altogether.
- Risk assessment, consent discussion, and a plan for monitoring and follow-up.
Skin type and timing can influence the decision. If the barrier is irritated, if active acne or infection is present, or if a patient has recently had another procedure, the doctor may delay treatment or choose a different route. In some cases, neither exosomes nor polynucleotides will be appropriate at that stage.
Monitoring matters because regenerative procedures often unfold over time. A doctor-led consultation therefore includes an explanation of likely treatment spacing, review points, and whether photography or serial assessment is useful for tracking response.
Pro Tip: For best results from polynucleotide injectables, follow your doctor’s prescribed aftercare and attend all scheduled review appointments.
What to Expect During Treatment: Process, Safety, and Outcomes
The treatment process begins before any product is used. Pre-treatment assessment, consent, and review of contraindications are part of the appointment, whether the plan involves an exosome treatment process or a polynucleotide procedure.
Preparation usually includes cleansing the skin, confirming the treatment area, and discussing what the session will involve. Topical anaesthetic may be used for some injectable procedures, depending on the area and the protocol.
During treatment, the experience differs according to the method selected. Polynucleotide injections are generally delivered into targeted areas using a clinical injection technique. Exosomes may be incorporated into a broader procedural plan, depending on the doctor-led protocol and the product indication.
Immediately afterwards, patients may notice redness, swelling, tenderness, or small marks at treatment sites. The exact pattern depends on the product, the delivery method, and the area treated. Post-treatment care is usually straightforward, but the doctor should still provide specific instructions on skincare, exercise, heat exposure, and timing of other procedures.
Outcomes are usually assessed over a series of appointments rather than a single session. Some treatments are planned as a course, with review after each stage to judge tissue response and whether the original goal remains appropriate. That measured approach matters more than chasing a fast visible change.
Pricing should be discussed factually because cost depends on the protocol, area treated, and whether treatment is standalone or part of a combined plan. Future Care Medical publishes medical aesthetics pricing for several doctor-led skin procedures, including Fotona 4D at £530.00, SylFirm X at £620.00, PicoSure Pro at £480.00, LDM at £140.00, Mark Vu at £65.00, and LED Dermalux at £90.00. Exosome and polynucleotide treatment costs should be confirmed in consultation where relevant to the proposed pathway.
Looking Forward: The Changing Role of Regenerative Treatments in Clinical Care
Regenerative skin treatments are attracting attention because they sit between traditional skincare and more invasive intervention. That position can be useful clinically, but it can also create confusion if the language around them becomes vague or inflated.
Evidence-based skin therapies depend on careful product selection, clear indications, and proper governance. Ongoing research may refine how exosomes and polynucleotides are used, which patients are most suitable, and which treatment combinations make sense within clinical innovation.
A few points are worth keeping in view:
- These treatments are medical options, not generic beauty procedures.
- Suitability is individual and depends on assessment, not trend.
- Medical oversight in aesthetics matters because product choice, timing, safety, and follow-up all affect decision-making.
The future of regenerative treatments will likely depend less on novelty and more on disciplined clinical use. Patients usually make the best decisions when they understand that exosomes and polynucleotides are tools with different roles, rather than rival labels for the same thing.
Request Pricing Information
Contact us for detailed, tailored pricing on exosome and polynucleotide treatments recommended for you.