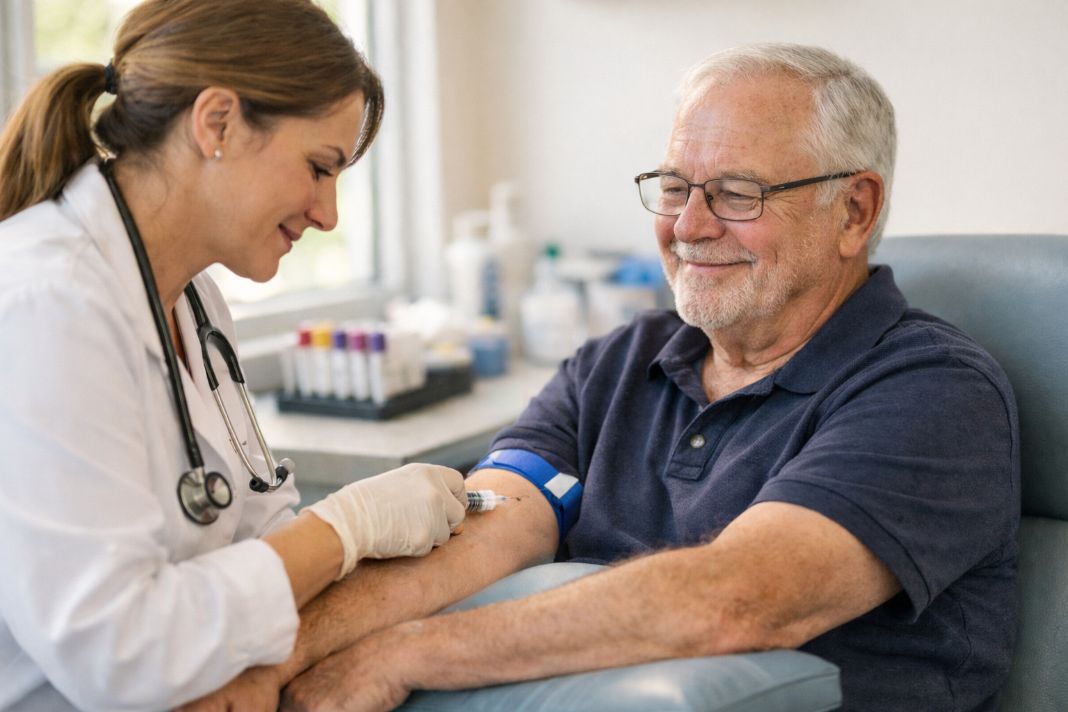
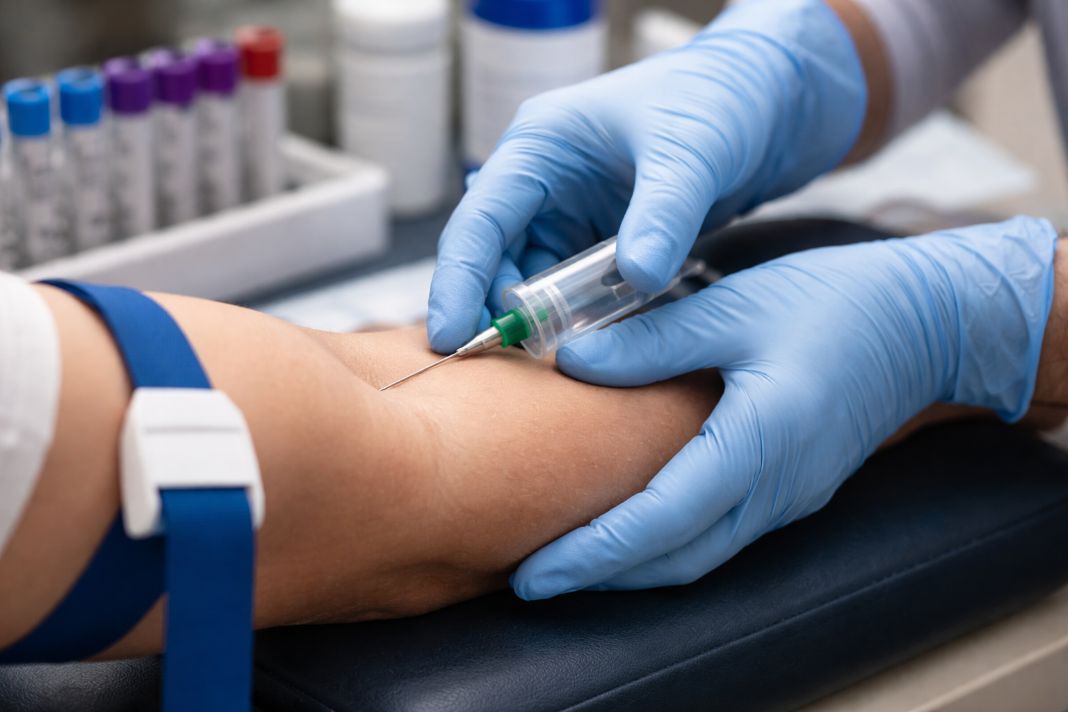
Which blood tests are worth considering in your 30s if you feel well?
A sensible starting point usually includes a full blood count, kidney and liver function tests, a lipid profile, and HbA1c. Beyond that, tests such as thyroid function, iron studies, vitamin D, hormone panels, or sexual health screening depend on symptoms, family history, lifestyle, and personal risk factors rather than age alone.
Many people in their 30s feel well, stay busy, and assume that screening can wait until later. Yet several common conditions change quietly at first, with blood markers shifting before symptoms become obvious in day-to-day life.
That is why blood screening in your 30s can be useful as part of a proactive health assessment. The goal is not to search for every possible problem. The aim is to build baseline health data, identify asymptomatic risk where it is clinically relevant, and make decisions early enough for intervention to be simpler.
Public guidance from bodies such as NICE and the NHS supports a risk-based approach rather than blanket testing for everyone. Primary care clinics and private medical clinics both use that principle, even if access, speed, and the structure of follow-up differ.
Some assumptions often get in the way:
- Feeling healthy means blood tests are unnecessary.
- Screening is mainly for people over 50.
- A single normal result means future checks are not needed.
- More tests automatically produce better answers.
A measured approach works better than either extreme. Routine blood work is most useful when it is chosen for a reason and interpreted in context, which leads naturally to the question of what belongs in an important panel.
Here's What We Have Covered In This Article
Core blood tests to consider: the important panel
A baseline screening panel in your 30s usually focuses on the tests most likely to reveal common, meaningful changes in health status. At Future Care Medical, structured blood panels are typically built around this kind of clinical logic rather than a long menu of tests with little relevance to the individual.
- Full blood count (FBC): This test looks at red cells, white cells, and platelets. It can point to anaemia, infection, inflammation, or other blood-related abnormalities.
- Liver function tests (LFTs): These measure enzymes and proteins linked to liver health. Results may be relevant if there is alcohol exposure, certain medication use, fatty liver risk, or unexplained symptoms.
- Kidney function tests (U&Es): Urea, electrolytes, and creatinine help assess kidney function and fluid balance. They are often included in standard health check bloods because kidney changes may be silent early on.
- Lipid profile: Cholesterol testing usually includes total cholesterol, HDL cholesterol, LDL cholesterol, and triglycerides. These results contribute to cardiovascular risk assessment.
- HbA1c: This reflects average blood glucose over the previous few months. It is widely used in diabetes screening and can identify raised blood sugar before diabetes is diagnosed.
Reference ranges matter, but they do not tell the whole story on their own. A result can fall within range and still prompt review if symptoms, family history, or previous trends suggest a closer look is needed.
Repeat testing depends on what the first panel shows. Someone with normal initial blood work and no strong risk factors may not need frequent retesting, whereas a person with borderline cholesterol, raised HbA1c, or a significant family history may need shorter test intervals.
Screening for metabolic and cardiovascular risk
Metabolic risk often develops without warning signs that are easy to notice. A person can exercise, work long hours, and feel generally fit while insulin resistance, unfavourable cholesterol patterns, or raised glucose begin to develop in the background.
Family history often changes the picture. If a parent or sibling has type 2 diabetes, high cholesterol, early heart disease, or high blood pressure, cholesterol testing and diabetes screening may be worth considering earlier and more regularly.
A focused metabolic health check often centres on a small group of blood tests and the risks they help clarify:
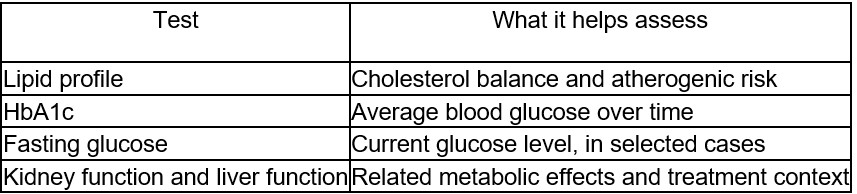
Risk calculators used in primary care can help place some results into a broader cardiovascular framework, although age in the 30s may keep calculated risk scores relatively low even when there are warning signs. That is one reason clinicians also look at weight pattern, blood pressure, smoking status, ethnicity, activity level, and family history rather than relying on a single number.
More advanced screening is not automatically necessary. A standard panel may be enough for one person, while another may need extra assessment because of obesity, previous gestational diabetes, polycystic ovary syndrome, a strong family history, or abnormal prior results. Clinics such as Future Care Medical often use that structured approach to risk identification so that testing stays proportionate to the individual in front of them.
Hormonal and thyroid function testing
Hormone and thyroid blood tests can be useful in your 30s, but they are usually guided by symptoms or a specific clinical concern rather than used as routine screening for everyone. Persistent tiredness, unexplained weight change, menstrual irregularity, fertility concerns, reduced libido, or changes in mood may justify a closer look.
Common situations that may prompt a thyroid blood test or hormone panel include:
- Ongoing fatigue that is not explained by sleep, workload, or illness
- Unexplained weight gain or weight loss
- Menstrual cycle changes or absent periods
- Fertility concerns
- Symptoms of low testosterone or other reproductive hormone imbalance
- Palpitations, heat intolerance, or feeling unusually cold
- Hair thinning or skin changes when paired with other symptoms
Thyroid function checks usually include TSH and, where appropriate, free T4. These tests help identify underactive or overactive thyroid function, including milder abnormalities that may need monitoring rather than immediate treatment.
Reproductive hormone screening varies according to the clinical question. Timing within the menstrual cycle can matter for some tests, and a single result may not be enough to explain a symptom pattern. In men, hormone testing may be considered if there are symptoms such as reduced libido, erectile dysfunction, infertility concerns, or loss of muscle mass. A GP consultation is usually the best place to decide which tests are relevant and when they should be taken, because interpretation depends heavily on context.
Pro Tip: If your first blood test panel is normal, save your results to compare against future screenings for helpful long-term insight.
Book a Personalised Blood Test Panel
Find out which blood tests are most relevant to your health profile by booking a tailored screening at Future Care Medical.
Screening for iron, vitamin D, and nutritional status
Iron deficiency and low vitamin D can both contribute to fatigue, poor concentration, and reduced physical resilience, but those symptoms are common and non-specific. Testing makes sense when the clinical picture suggests a genuine possibility rather than as an automatic add-on.
A useful way to think about nutritional blood panel requests is to match symptoms and risk factors with likely deficiencies.
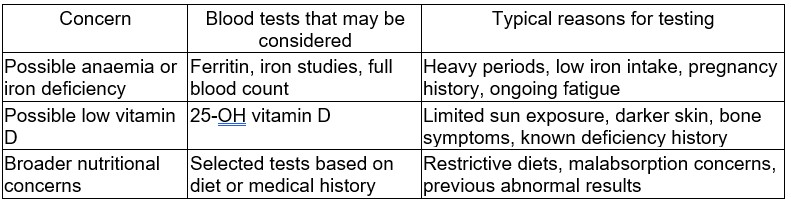
Ferritin is often central when checking for anaemia linked to iron deficiency, because it reflects iron stores. Iron studies may be added to clarify a more complex picture, particularly if inflammation or chronic illness could affect interpretation.
Vitamin D screening is sometimes overused. Many adults in the UK are advised about supplementation without necessarily needing a blood test first, especially when there are no symptoms or risk factors. By contrast, someone with bone pain, recurrent low levels, osteoporosis risk, or a condition affecting absorption may benefit from a measured assessment before treatment decisions are made.
Sexual health and infection screening
Sexual health blood tests are a routine part of adult healthcare, including in your 30s. Symptoms are not required for screening, because several infections can remain silent for long periods.
Blood-based sexual health screening may include:
- HIV
- Hepatitis B
- Hepatitis C
- Syphilis serology
Need, timing, and frequency depend on exposure risk. A new partner, multiple partners, sex without barrier protection, previous infection, or a partner’s known diagnosis can all affect the decision to test. Some people also choose regular STI screening as part of their routine healthcare, particularly if their circumstances change over time.
Confidentiality matters here. Sexual health clinics and private GP services generally work within clear systems for consent, privacy, result reporting, and any necessary follow-up. If a result is positive, management may include confirmatory testing, treatment, advice on partner notification, and referral where appropriate. A private sexual health check should feel routine and structured, which means that stigma has no useful role in the process.
How blood test results inform ongoing health decisions
Blood tests are rarely the end of the story. A result becomes useful when it is reviewed alongside symptoms, blood pressure, weight pattern, medication use, family history, and previous readings.
One person may have a mildly raised cholesterol level that leads to lifestyle review and repeat testing in several months. Another may have a normal result that simply serves as baseline data for future comparison. A third may need more investigation because a pattern across several markers points to a wider issue.
Follow-up after blood tests often includes one or more of the following:
- Repeat testing after a defined interval
- A GP consultation to interpret results in clinical context
- Additional tests if a finding needs clarification
- Monitoring through a broader health screening package
- Treatment or referral if an abnormality has clear significance
Trend monitoring is especially helpful. A single result offers a snapshot, whereas repeated measurements can show direction of travel. That distinction matters for glucose control, lipid levels, thyroid function, iron stores, and several other markers commonly included in ongoing health monitoring.
At Future Care Medical, blood test review may sit within a wider care pathway that includes GP assessment, follow-up protocols, and broader screening where indicated. The principle is straightforward: numbers do not make decisions on their own, and good interpretation depends on both timing and context.
Pro Tip: When booking blood tests, provide your doctor with information about family history and any subtle symptoms to ensure the right panel is chosen.
Rethinking health screening in your 30s: common misconceptions and forward-looking insights
The idea that meaningful screening starts only in later life is one of the most persistent health screening myths. In reality, your 30s are often the decade when risk begins to separate more clearly between individuals, even if most people still feel broadly well.
A few misconceptions are worth dropping:
- Blood test misconceptions often come from treating age as the only factor that matters.
- Low personal risk should be assessed, not assumed.
- Normal results are useful, but they do not remove the need for future review if circumstances change.
- Preventative health in your 30s is not the same as testing for everything available.
NICE guidelines and primary care frameworks generally support proportionate screening based on symptoms, family history, and identifiable risk. That approach can feel less dramatic than broad testing, yet it often gives better information and creates fewer false alarms.
Attitudes to screening may change as work patterns, reproductive plans, body weight, exercise habits, and family history become more relevant over time. The most useful mindset is neither complacent nor obsessive. It is informed, selective, and willing to use blood tests as one part of a longer view of health.