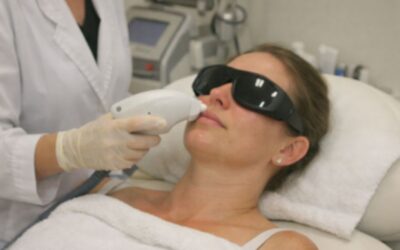
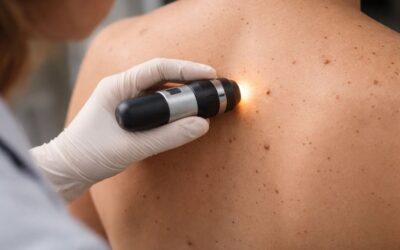
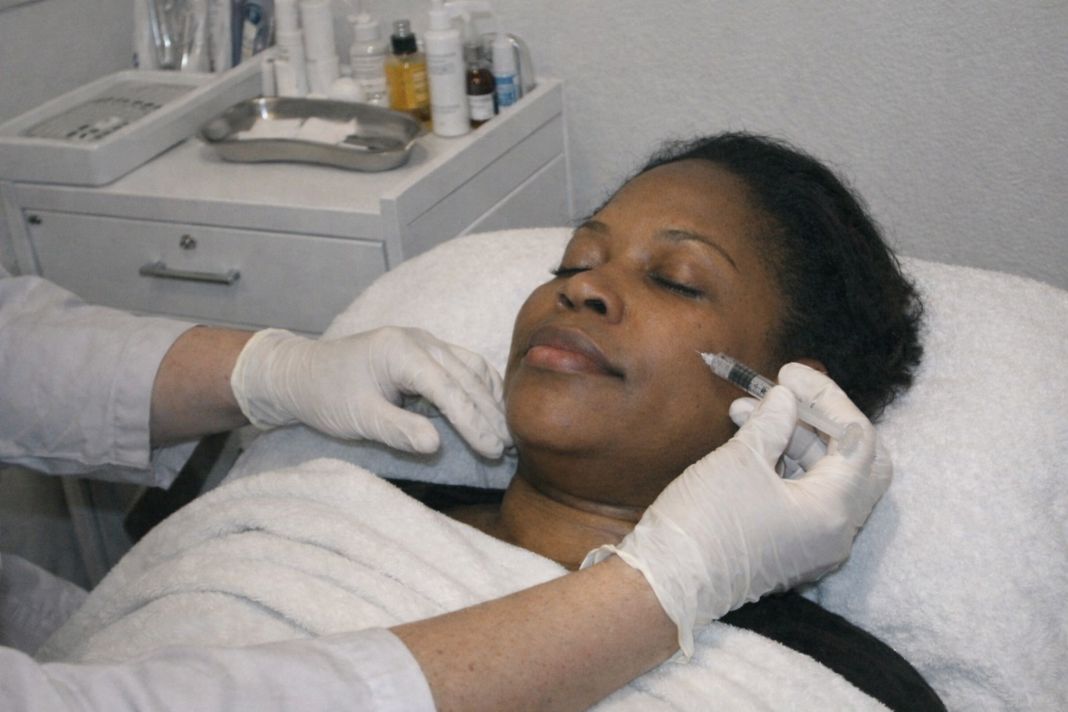
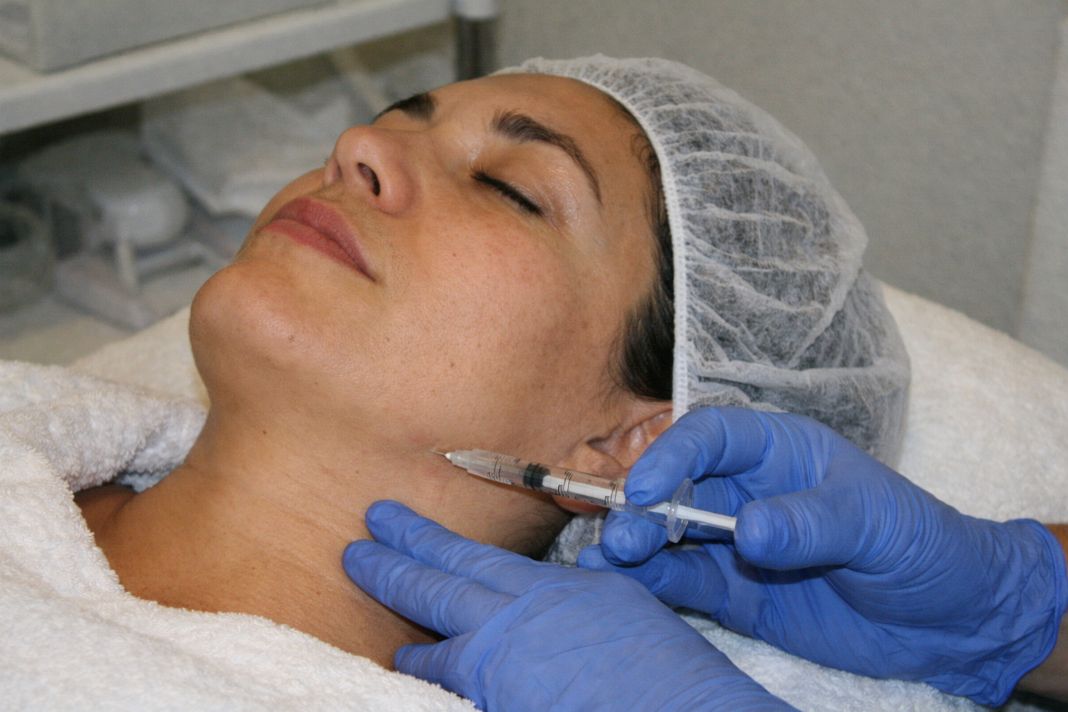
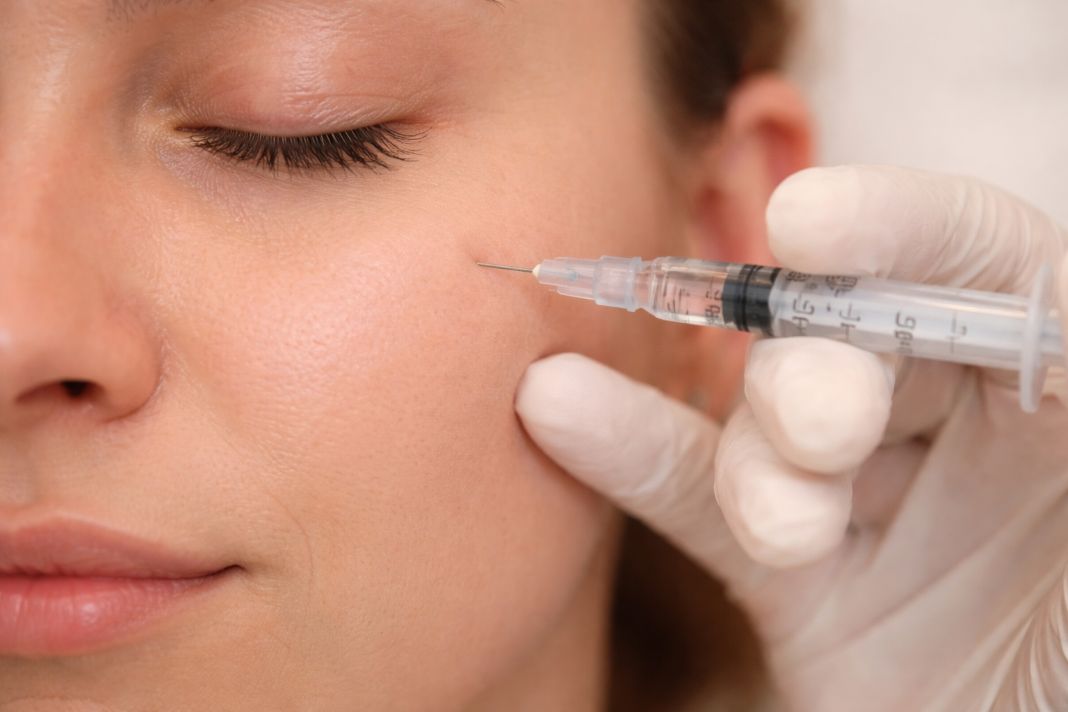
How do medical aesthetic clinics differ from non medical providers in terms of safety?
Medical aesthetic clinics are distinguished by clinical oversight, regulatory requirements and the qualifications of their practitioners, which combine to offer structured safety measures beyond those typically found in non medical clinics. Their strong protocols, trained personnel, and adherence to formal governance standards contribute to a regulated environment designed to protect patients.
Here's What We Have Covered In This Article
Understanding the Difference Between Medical and Non Medical Aesthetic Clinics
Knowing whether an aesthetic clinic is “medical” or “non medical” shapes your expectations around safety, treatment quality and legal protections. The term “medical” in this setting refers to clinics or providers working under strict clinical frameworks, led by doctors or registered healthcare professionals who must comply with statutory regulation.
Here are key differences between medical and non medical aesthetic clinics:
- Clinical Oversight: Medical clinics must have medical directors and are subject to regular inspection by bodies such as the Care Quality Commission (CQC).
- Regulated Practitioners: Treatments are delivered by doctors or allied health professionals registered with the General Medical Council (GMC) or the Health and Care Professions Council (HCPC).
- Treatment Scope: Medical clinics can provide prescription-only medicines and advanced procedures requiring clinical diagnosis.
- Protocols and Governance: Medical settings require formal consent processes, incident reporting and full patient records.
By contrast, non medical clinics tend to be run by practitioners without medical registration. They may offer treatments based on aesthetic training courses and operate outside clinical governance frameworks. Public perception of what is “medical” can be shaped by branding or titles. However, only clinics registered with the relevant regulatory bodies are considered medical in a legal sense. This distinction carries direct implications for patient safety and recourse.
Pro Tip: Check a provider’s CQC registration online for reassurance about regulatory oversight and inspected standards.
Book a Medical Consultation
Gain peace of mind by booking your initial consultation with our qualified medical team for personalised aesthetic advice.
Safety Protocols and Clinical Governance in Medical Aesthetic Clinics
Strong governance and well-defined protocols underpin the safe delivery of aesthetic treatments in medical clinics. Safety is maintained through layers of process and oversight, which together form the foundation of patient protection.
Clinical Governance Frameworks Medical clinics adhere to frameworks set out by regulatory bodies such as the CQC. These frameworks outline how quality and safety should be managed, with accountability assigned to a medical director.
Consent and Assessment Protocols A detailed medical history, risk assessment and informed consent are mandatory before any treatment. This ensures patients fully understand the nature, benefits and potential risks of a procedure.
Incident Reporting and Risk Management Should adverse events occur, medical clinics maintain reporting systems to investigate and address these incidents. Processes include documentation, review and escalation if required.
Infection Control and Patient Records Sterile environments, strict hygiene routines and proper waste disposal are standard. All treatments and follow-up communications are documented within secure patient records for traceability and accountability.
Safety Audits Regular internal or external audits assess compliance with relevant standards, supporting a culture of continual improvement.
This structured approach reassures patients that clear mechanisms exist for decision-making and safety monitoring, shaping a safer overall environment.
Practitioner Qualifications and Training Standards
Who delivers aesthetic treatments directly affects safety. Medical clinics, by definition, engage practitioners registered with recognised medical regulators and oversee their work within multidisciplinary teams.
Medical Clinics
- Treatments are provided by doctors (GMC-registered), nurses or allied health professionals (HCPC-registered).
- Practitioners must complete recognised medical qualifications and engage in ongoing training, including revalidation and professional development.
- Clinical staff participate in regular case reviews and team meetings to discuss complex scenarios or complications.
Non Medical Clinics
- Treatments may be delivered by individuals with aesthetic training certificates but no recognised medical qualification.
- Limited requirements exist for ongoing professional development.
- Escalation in case of complications may be restricted, especially when prescription medicines or advanced intervention are required.
The difference in qualifications is significant. Medical clinics offer not just advanced treatment skills but also escalation pathways in complex or emergency scenarios. Patients can check a provider’s registration status easily using the GMC or HCPC online registers, which increases transparency and trust.
Risk Management and Handling of Complications
What happens if a procedure does not go according to plan? Prompt, structured responses to complications are a cornerstone of medical clinic safety.
Immediate Response and Escalation Medical clinics keep emergency medicines and equipment available and have protocols for immediate intervention. Registered clinicians can prescribe medicines if needed and initiate rapid referral to hospital care if a situation escalates.
Documentation of Adverse Events Incidents are recorded in detail, providing an audit trail for internal learning and supporting any patient complaint or investigation if necessary.
Follow-Up and Monitoring Patients who experience complications receive structured follow-up, ensuring ongoing monitoring and access to further treatment if required.
By comparison, non medical clinics may not be able to prescribe medicines or activate escalation to a multidisciplinary team or hospital. This limitation can delay appropriate management of serious complications.
Pro Tip: During your consultation, ask for detailed information about aftercare and escalation procedures in case of complications.
Regulatory Oversight and Legal Responsibilities
Regulation shapes the responsibilities and accountability of aesthetic providers.
Statutory Regulation (Medical Clinics)
- Clinics offering certain medical treatments are required to register with the CQC.
- Inspections assess compliance and the results are made publicly available.
- Registered professionals must adhere to codes of conduct set by the GMC or HCPC.
Voluntary Registers (Non Medical Clinics)
- Many non medical clinics participate in voluntary schemes with varying standards and no statutory backing.
- Inspection and legal oversight are less rigorous or absent.
Inspection and Complaints Medical clinics undergo announced and unannounced inspections, with findings accessible on the CQC website. Patients can make formal complaints to the clinic or escalate to the CQC, GMC, or HCPC.
By contrast, those treated in non medical clinics may have limited recourse if issues arise, particularly in relation to medical negligence or standards of care.
Patient Experience: What to Expect in a Medical Aesthetic Clinic
The patient process in a medical aesthetic clinic is shaped by structure and clarity at each step.
- Initial Consultation A detailed clinical consultation involves history taking, assessment and discussion of expectations. Risks and benefits are outlined by a medically qualified practitioner.
- Informed Consent Written consent is obtained, with time for questions and an explanation of the treatment plan.
- Treatment Procedures are delivered within a clinical environment, following strict hygiene and safety standards.
- Aftercare Patients receive clear post-procedure instructions and a direct contact point for questions or concerns.
- Follow-Up A review appointment or remote check-in may be arranged to ensure recovery and address any late-onset effects.
Future Care Medical, for example, operates this structured pathway for all medical aesthetic treatments, prioritising medical oversight and patient clarity throughout.
In non medical clinics, certain steps such as risk assessment or aftercare follow-up may be less formalised, with variable adherence to consent and patient documentation standards.
Making an Informed Choice: Key Questions to Ask Before Treatment
Selecting an aesthetic provider requires careful consideration of safety, qualifications and regulatory status. Patients can take an active role by asking direct questions before undergoing treatment.
Safety and Quality Checklist
- Is the clinic registered with the Care Quality Commission (CQC)?
- What are the practitioner’s qualifications and which professional body are they registered with?
- What protocol does the clinic follow for patient consent and risk assessment?
- How does the clinic manage complications, and can they prescribe emergency medicines if required?
- What aftercare and follow-up are provided, and who should be contacted with concerns?
- Are treatment costs, such as consultation fees or package prices, clearly stated and transparent?
Understanding the answers to these questions helps patients set realistic expectations and establish whether a provider meets their safety requirements. Future Care Medical openly lists practitioner credentials and publishes its GP and aesthetic consultation pricing for transparency, supporting informed decision-making.
A clear distinction exists between medical and non medical providers in both structure and governance. Patients considering aesthetic treatments in Central London or beyond are encouraged to prioritise regulatory registration, formal clinical pathways and accessible escalation routes for best safety and peace of mind.
Learn About Our Safety Protocols
Explore the clinical governance, audit, and aftercare measures we have in place to protect your wellbeing.